Scientists from Waseda University, the National Defense Medical College, and the Japan Science and Technology Agency have developed a new bioadhesive, wirelessly-powered light-emitting device which has the potential to improve the treatment of cancers in delicate organs.
Conventional photodynamic therapy causes cancer cells to die by using photosensitizing agents, these agents localize in tumors and activate when they are exposed to a specific wavelength of light. Though recently, low-dose and long-term photodynamic therapy (metronomic photodynamic therapy, mPDT) has shown that it could help in treating cancers in internal organs.
But a main problem with mPDT is that- since the light intensity is extremely low (1/1000 of the conventional method)- it makes it impossible to achieve the the antitumor effect if the light source shifts even slightly away from the tumor, which makes the illumination insufficient.
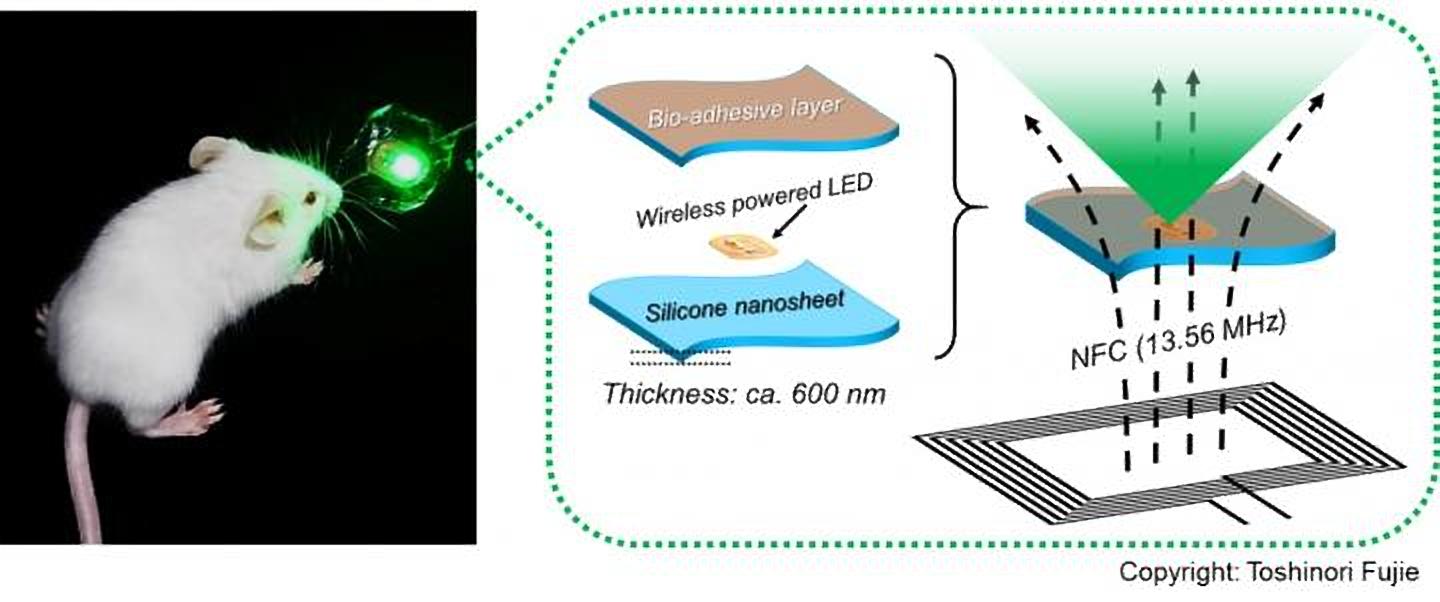
“To address this issue, we have developed a wirelessly-powered optoelectronic device that stably fixes itself onto the inner surface of an animal tissue like a sticker with bioadhesive and elastic nanosheets, enabling a continuous, local light delivery to the tumor,” said Toshinori Fujie, who is the associate professor of biomedical engineering at Waseda University.
This study was published recently in the journal Nature Biomedical Engineering.
The nanosheets have been modified with the mussel adhesive protein-inspired polymer polydopamine, which has the ability to stabilize the device onto a wet animal tissue for more than 2 weeks without any surgical suturing or medical glue. The light-emitting diode chips present in the device are powered wirelessly by near-field-communication technology.
To test its effectiveness, the researchers implanted tumor-bearing mice with the device and injected them with a photosensitizing agent (photofrin) and then exposed them to red and green light, which had nearly 1,000-fold intensity lower than the conventional PDT approaches, for a period of 10 days. The findings of the experiment show that the tumor growth was considerably reduced overall, especially under green light, with the tumor in some mice getting completely eradicated.
Associate Professor Fujie explained, “This device may facilitate treatment for hard-to-detect microtumors and deeply located lesions that are hard to reach with standard phototherapy, without having to worry about the risk of damaging healthy tissues by overheating. Furthermore, because the device does not require surgical suturing, it is suitable for treating cancer near major nerves and blood vessels, as well as for organs that are fragile, that change their shape, or that actively move, such as the brain, liver, and pancreas.”